The A, B, Cs of the Governance of Antimicrobial Resistance – What it is and Why it Matters for Human and Animal Health
by GLID students Sabrina Barrett, Matt Boyce, and Jordan Cuevas
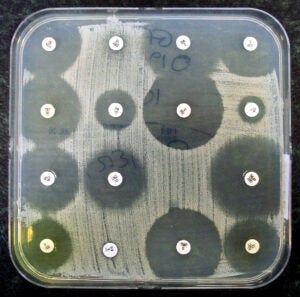
Image Courtesy Dr. Graham Beards via Creative Commons license.
The development of antimicrobials – such as antibiotics, antivirals, antiparasitics, and antifungals – arguably represents one of the greatest successes of modern medicine. These medicines have allowed humans to combat the scourges of some of the deadliest diseases in history and reduced complications stemming from now commonplace medical procedures.
Still, our time with these technologies may be waning. Antimicrobial resistance (AMR), or the ability of pathogens to resist these technologies, threatens the effectiveness of our medicines and alludes to a reality defined by the inability to prevent infections. Such a development could jeopardize our ability to not only treat infectious diseases but also impact protocols for other ailments whose current treatments frequently leave patients immunocompromised (such as cancer, arthritis, and Crohn’s Disease) and procedures that use antimicrobials to prevent infection prophylactically or as treatment (such as surgery). Indeed, the threat posed by AMR is so great that in 2019, the World Health Organization listed it as one of the top-ten threats to health – placing it in company with other health concerns like climate change, HIV, and pandemic influenza.
AMR is a natural phenomenon that occurs as pathogens gradually evolve. However, human activities such as the inappropriate use of antimicrobials in people, animals, and in the environment have exacerbated the problem by placing selective pressure on the microbes to develop and disseminate resistance. Accordingly, in 2015 the Global Action Plan on Antimicrobial Resistance was adopted at the World Health Assembly. Many countries have subsequently developed, revised, and updated their national action plans to better combat the threat of AMR.
But because the use of antimicrobials is so pervasive in our society, addressing the challenges posed by AMR will require intersectoral action and strong leadership across a multitude of levels. Accordingly, while good governance and mechanisms for coordinating policy across sectors will be central to successfully combating the serious and global threat of AMR, it also represents a major challenge.
… because the use of antimicrobials is so pervasive in our society, addressing the challenges posed by AMR will require intersectoral action and strong leadership across a multitude of levels.
Defining the concept of governance is an arduous task. When done well, governance is not synonymous with government, but rather includes other societal groups and considers how these groups make decisions and interact with the general public. For the purposes of this blog, we will consider the World Health Organization’s 2002 definition of governance that outlines the closely related concept of stewardship according to six key domains: (1) generating knowledge, (2) formulating strategic policy direction, (3) ensuring tools for implementation (i.e., powers, incentives, and sanctions), (4) building coalitions and partnerships, (5) ensuring a fit between policy objectives and structure and culture, and (6) ensuring accountability.
Governance of antibiotic use in humans
The period between 1950-1970 was coined the “Golden Era of Antibiotics,” however no new antibiotic classes have been discovered since then. Over the last 50 years, the bacteria that we encounter regularly have been constantly exposed to a rotation of the same antibiotics and have developed the ability to resist them. Despite the fact that gradual resistance development is natural, human activities have escalated the speed with which resistance has evolved in bacteria due to the overuse and misuse of antibiotics. Accordingly, in order to slow down or combat the realities of AMR, governance of antibiotic use in humans must be made a priority while considering the following:
(1) Generating knowledge
There is a need for education both among patients and the general public regarding the appropriate use of antibiotics. Emphasis on infection prevention behaviors (personal hygiene, immunization, etc.) as well as education on proper and informed health seeking behavior is key to ensuring a systematic move away from overdependence on antibiotics. Providers should receive medical education on the rational use of antibiotics and the containment of antibiotic resistance. Providers should also act as educators for their patients and community regarding antibiotic use and the importance of adherence to prescribed treatments.
(2) Formulating strategic policy direction
The One Health approach recognizes that human health is intrinsically tied to the health of animals and our shared environment. Goals and policies structured with One Health allow for a systematic approach that incorporates human use of antibiotics with other factors that impact AMR development. Applying a One Health perspective in policy development could also ensure international cooperation as all countries will adhere to the same principles.
(3) Ensuring tools for implementation
Establishing the capacity to detect, analyze, and report antibiotic resistance is a priority. This surveillance technology will allow for evidence-based decision making nationally and internationally. It is also a priority to incentivize the development of new therapeutics to counter AMR, including new, next-generation, and other alternatives to antibiotics, vaccines, and affordable, rapidly deployable, point-of-need diagnostics.
(4) Building coalitions and partnerships
Establishing and promoting international collaboration and public-private partnerships will be key in combating AMR in humans as failure to adhere to new standards undermines the entire effort. The global challenge of AMR requires coordination that spans beyond regional reform. Coordinated efforts must be made across borders in order to ensure lasting change.
(5) Ensuring a fit between policy objectives and structure and culture
Countries with national systems in place to track and combat AMR must support other countries in developing and implementing national plans and strategies to combat AMR. This support should take into account the current infrastructure, capabilities, and culture of the country or region being assisted in order to ensure lasting change.
(6) Ensuring accountability
Establishing direct incentives through managerial control in a top-down system could help to ensure accountability among healthcare workers. Public release of data regarding AMR status and recent outbreaks may also help to ensure accountability as well as ensuring that the public is aware of the seriousness of the issue, therefore also holding them accountable in maintaining their duties to adhere to treatment and practice appropriate health-seeking behaviors.
Governance of antibiotics use in livestock and companion animals
The use of antibiotics in livestock farming and companion animals represents another large contributor to the growing problem of AMR. Although the extent to which this use contributes to AMR remains unknown, addressing the issue of AMR within humans cannot be done without addressing similar issues within the animal sector. Thus, governance also plays a large part in the regulation of and education about antibiotic usage in animals. Education of the general public, veterinarians, and farmers, should decrease the misuse of antibiotics in livestock and companion animals, resulting in decreases in antibiotic resistance.
(1) Generating Knowledge
One of the major issues regarding animal and livestock antibiotic use is the lack of information surrounding prescriptions and distribution. The education of veterinarians and farmers is vital for combating this issue and slowing down the increasing bacterial resistance to antibiotics. Antibiotic providers should be given the necessary knowledge to understand when, and how much, to prescribe. In addition to educating people who work closest to animals, it is essential to educate and be transparent with the general public about what goes into their food, and how it can affect them.
(2) Formulating strategic policy direction
As previously stated, a multidisciplinary One Health approach is essential to countering AMR. This holistic approach is necessary, as the use of antibiotics must be limited in all sectors. The injudicious of antibiotics in the animal sector pertains to the growing resistance in humans, and the responsible governmental agencies (e.g., the United States Food and Drug Administration and United States Department of Agriculture) must work to incentivize pharmaceutical companies and prescribers to limit antibiotic use.
(3) Ensuring tools for implementation
Data for monitoring antibiotic use in animals is extremely limited and difficult to collect. Currently, antibiotic sales by pharmaceutical companies are used to track and estimate the amount of antibiotics given. Creating a database where this information can easily be found is essential for understanding the contribution of farming and companion animal antibiotic use to antibiotic resistance.
(4) Building coalitions and partnerships
Fostering partnerships between the government and veterinarians and pharmaceutical companies is also of importance. These collaborations could work to promote the development of novel technologies and approaches to address the threats posed by AMR.
(5) Ensuring a fit between policy objectives and structure and culture
Through education of the general public, and compliance of veterinarians and pharmaceutical companies, limiting antibiotic use in animals is possible. As the general public becomes aware of the importance of this issue, progress will be made regarding the misuse and overuse of antibiotics.
(6) Ensuring accountability
Holding the government and pharmaceutical companies accountable for educating medical professionals represents one way to decrease inappropriate antibiotic prescriptions, and subsequently antibiotic resistance.
Building a Successful Response to AMR
While our understandings of AMR remain relatively limited, what is clear is that AMR is occurring in every corner of our world – compromising our collective ability to treat bacterial diseases and threatening other advances in public health and medicine. Addressing these issues will require substantial amounts of time and resources and joint, intersectoral action will be necessary for coordinating efforts. Accordingly, the governance of AMR, in both the human and animal health sectors, represents a cornerstone in an urgently needed response to a dire public health challenge.